Wet brain is the more colloquial term for a particular brain disorder known as Wernicke-Korsakoff syndrome. There are medical circles that also alternatively use the terms Wernicke’s encephalopathy and Korsakoff’s syndrome in place of a wet brain, as these two conditions are believed to occur simultaneously. There are those who also believe that the two different terms are simply two parts of the same condition, where Wernicke’s encephalopathy is the acute phase while Korsakoff’s syndrome is the chronic stage.
Carl Wernicke, one of the people after whom the disease is named, was a German physician, psychiatrist, and neuropathologist. In 1881, he made a startling and horrific observation in three patients, all of whom manifested eye movement paralysis, ataxia (a disorder that causes difficulties in coordination, balance, and speech), and confusion.
All three patients eventually fell into a coma and died. Two of the patients, who were incidentally male, had an alcohol use disorder. The other patient, a female, had ingested sulfuric acid which caused her to vomit continuously. During an autopsy, all three patients had very similar brain lesions, which were largely held to be the main cause of the symptoms and eventual death of all three. Even more indicative of the highly damaging nature of the condition, the brains of all three people were found to have atrophied (degenerated and shrunk).
These three deaths seemed to foreshadow the trend of the disease, as men have been documented as being more particularly susceptible to developing wet brains than women.
Six years later, Russian neuropsychiatrist Sergei Sergeyevich Korsakoff announced his “discovery” of psychosis polyneuritic, which eventually became known as Korsakoff’s psychosis, Korsakoff’s dementia, and later still, Korsakoff’s syndrome.
However it is called, it is a severe and life-threatening disorder that typically begins from a deficiency in thiamine, a vitamin that belongs to the B complex group. It is most pronounced in people who have an alcohol use disorder, and to a lesser extent, those who suffer from chronic vomiting or malnutrition. Alcohol interferes with the body’s ability to absorb vitamin B1, which is why people who have a history of alcoholism have a higher chance to develop a wet brain.
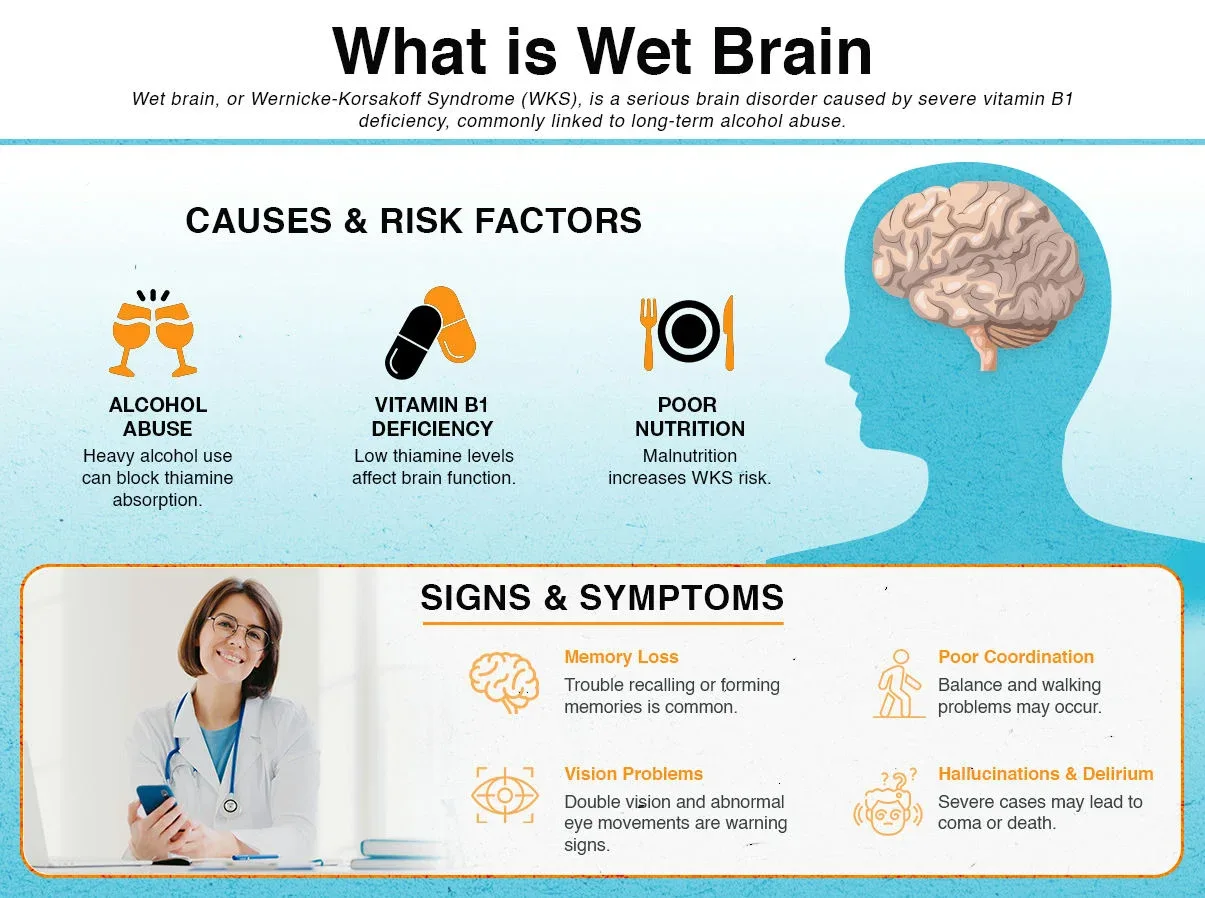
What Are the Symptoms of a Wet Brain?
As it directly affects the brain, the wet brain tends to create behavioral changes in the person. These behavioral changes, however, are not immediately identifiable as being symptoms of the wet brain due to the fact that some other health conditions could also have the same manifestations. Some of the symptoms have even been seen in people who have suffered from some form of head trauma, which makes symptom association quite difficult. The wet brain is known to manifest different symptoms in two distinct stages:
First Stage – Wernicke’s Encephalopathy
Stage 1 is known as the onset of Wernicke’s encephalopathy and may manifest the following symptoms:
- Sudden impaired mental ability
- Confusion
- Impaired muscle coordination
- Leg tremors
- Abnormal eye movements
- Diplopia (double vision)
- Droopy eyelids
- Loss of consciousness
- Coma
Wernicke’s encephalopathy, while typically known to come with severe psychological and physical symptoms, is also held to be temporary. It should be noted, however, that once the condition has been established to be Wernicke’s encephalopathy, medical attention should immediately be sought, because if it is left untreated, it could rapidly shift into the more lethal second stage.
While the wet brain is generally held to have no cure, treatment with thiamine supplements during the first stage is held to alleviate the symptoms, and more importantly, prevent the degeneration of the first stage into the lethal second stage. The high doses of thiamine, however, will only work if it is administered during the early phase of the first stage. Thiamine supplements will have no effect once the condition degenerates into the second stage.
Second Stage – Korsakoff’s Psychosis
The second stage is after Wernicke’s encephalopathy and is known as Korsakoff’s psychosis, held to be the lethal stage, as it occurs when the first stage is left untreated, and severe damage has already been done to the brain.
Korsakoff’s psychosis is persistent, chronic, and irreversible. Some refer to this phase as alcoholic dementia, as it mimics the manifestations of dementia and is brought about by severe alcoholism.
- Impaired memory
- Inability to form new memories
- Vivid hallucinations
- Confabulation (“remembering” events that did not happen)
- Fatigue
- Delirium
- Inability to focus or pay attention
- Loss of consciousness
- Coma
- Death
The National Institute on Alcohol Abuse and Alcoholism has released data pointing to the fact that 80% to 90% of alcoholics who suffer from Wernicke’s encephalopathy could also develop Korsakoff’s psychosis.
It should also be noted that while alcohol abuse is the leading cause of wet brain, other conditions are also known to inhibit the body from properly absorbing thiamine, and likewise lead to the wet brain. These conditions include:
- Advanced stages of cancer
- Kidney failure
- Liver disease
- Long-term dialysis
- Thyrotoxicosis (a condition that causes high thyroid hormone levels)
- A heart condition that requires diuretic therapy treatment
- Extreme or chronic nausea with vomiting (anorexia)
- Severe malnutrition
There are also people who do not have any of these conditions but have an inherent difficulty in absorbing or processing certain vitamins or nutrients. It is essential to seek a doctor’s assessment if this peculiarity is present. Therefore, whatever supplements or infusions could be found and administered before the lack of the nutrient or vitamin reaches a critical level and lead to adverse conditions, such as a wet brain.
The danger of a wet brain lies in the fact that a proper diagnosis cannot be made on the person as the symptoms are quite similar to many of those experienced during alcohol withdrawal. The only time a proper diagnosis could be reliably done is when the person is already in the recovery phase of alcohol abuse rehab, and this conflicts with the need to detect the possibility of the wet brain as early as possible.
Can Wet Brain Be Treated?
 Treatment for the wet brain can only be done if it is identified in its early stage. The problem with this, however, lies in the fact that proper identification is difficult to conduct as most symptoms of the first stage of the wet brain mimic that of alcohol withdrawal.
Treatment for the wet brain can only be done if it is identified in its early stage. The problem with this, however, lies in the fact that proper identification is difficult to conduct as most symptoms of the first stage of the wet brain mimic that of alcohol withdrawal.
Even with early identification, however, there is always a chance the condition could devolve into the lethal second stage should alcohol be consumed once more, or if any dietary changes further prevent the body from receiving thiamine. The only treatment being used thus far is the administration of high doses of thiamine to compensate for the lack of it in the body.
A balanced diet is also highly recommended as malnutrition is a major contributing factor to the development of the wet brain and to its worsening. Food items such as oranges, milk, spinach, pork, and soybeans are high in thiamine content, and as such, should be included in the diet. Observed treatments indicate that adequate administration of thiamine led to a significant and noticeable improvement in the person’s mental status in as little as two to three weeks of continuous therapy.
Complete abstinence from alcohol intake is essential so that the condition does not worsen should the person already have it. Abstinence is still highly recommended even if the person appears to have completely recovered from the ill effects of the first stage, as the body might still be vulnerable to thiamine depletion.
Considering the nature of the wet brain, doctors advise the only option that a person does need to develop is prevention. Anyone who is at high risk of not being able to absorb thiamine due to any reason is highly advised not to consume alcohol. People with eating disorders should also be assessed if their thiamine levels have dropped to dangerously low levels, as this is also one way of developing a wet brain.
People who have other pre-existing conditions that could also compromise their ability to absorb thiamine should have a doctor assess them to know if they need to take thiamine supplements. There are also some people who have a particular quirk in their physical makeup where they are unable to process or absorb any other vitamin or mineral, and in some cases, some nutrients, when they take a certain potent medication.
This apparently internal conflict where the body is unable to process or absorb other things while processing a potent medication could also contribute to a lack of thiamine, among other essential things that the body might need. If this is the case, a doctor could suggest other ways where the body could still receive the needed vitamins and nutrients, just so the lack does not lead to adverse effects.
We Take the Matter of Care and Recovery Seriously Here
We always consider the process of recovery to be a very delicate thing. It doesn’t matter if the person appears to be strong enough to recover quickly or far better than others; we consider everyone’s recovery crucially, so we exercise the utmost care and attention to them. We don’t take chances with your recovery at Free By The Sea in Ocean Park, Washington. Neither should you. Contact us today.


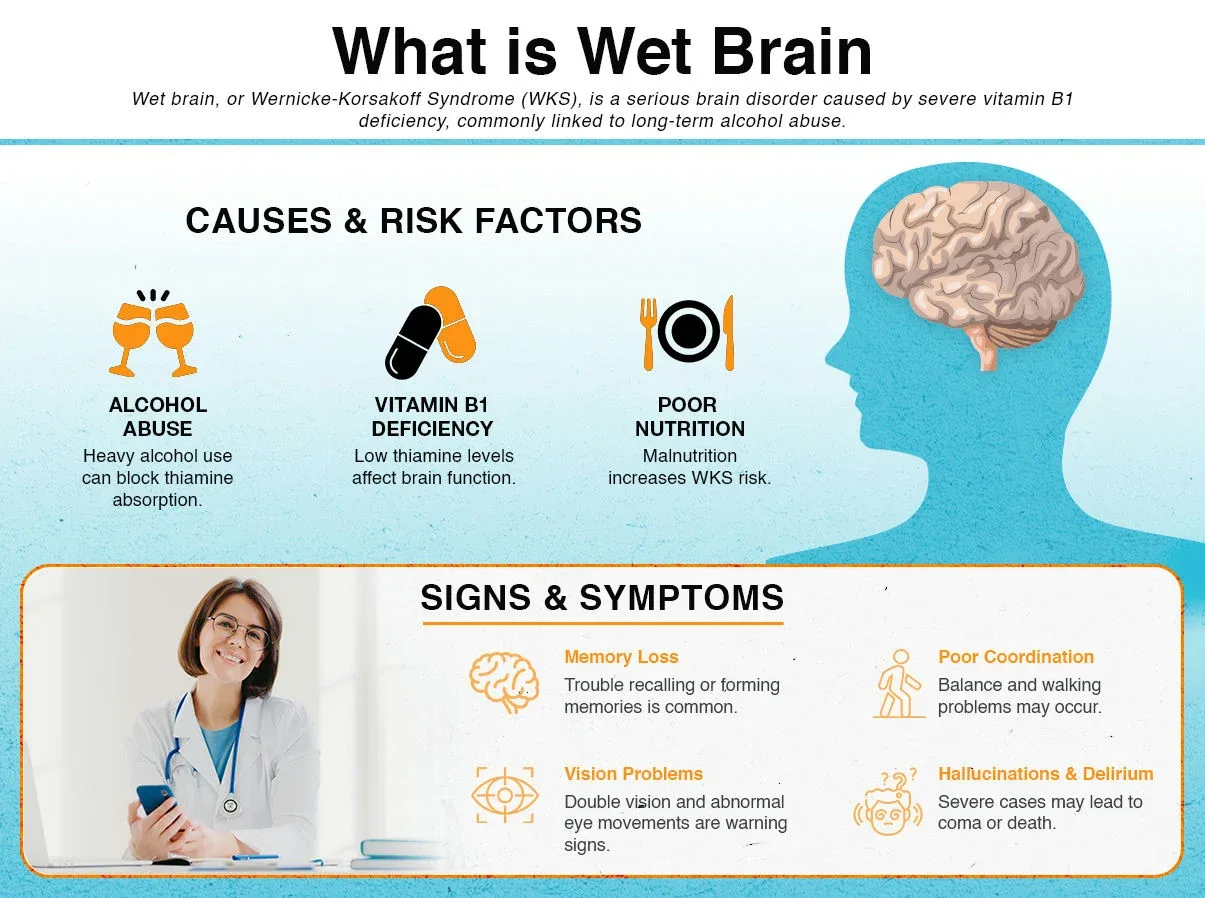
 Treatment for the wet brain can only be done if it is identified in its early stage. The problem with this, however, lies in the fact that proper identification is difficult to conduct as most symptoms of the first stage of the wet brain mimic that of alcohol withdrawal.
Treatment for the wet brain can only be done if it is identified in its early stage. The problem with this, however, lies in the fact that proper identification is difficult to conduct as most symptoms of the first stage of the wet brain mimic that of alcohol withdrawal.




















