Can Alcohol Withdrawal Cause Seizures?
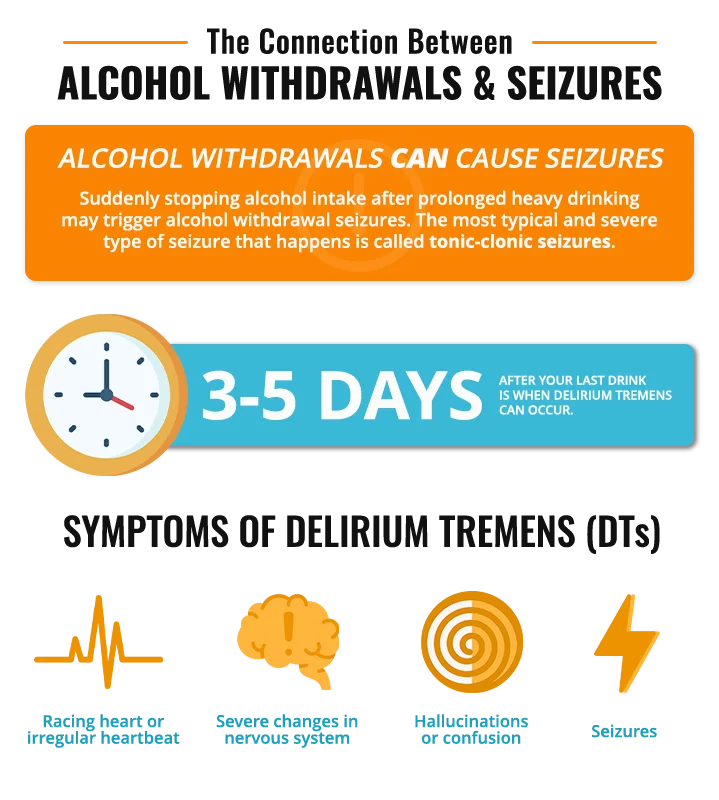
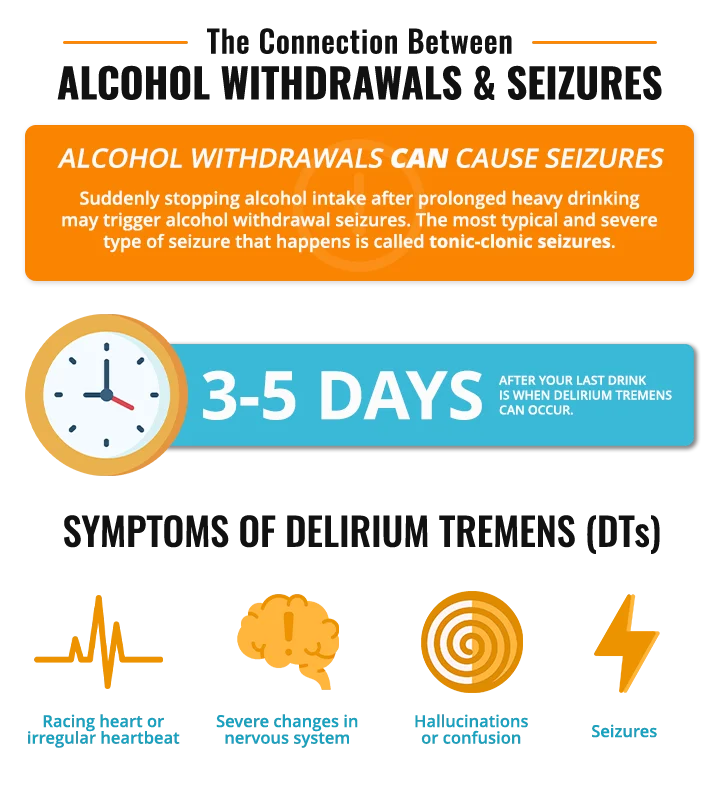
Yes. Alcohol withdrawal seizures can occur within 8 to 24 hours after heavy drinking is stopped. These seizures are typically generalized and may happen as a single seizure or in clusters over several hours. Sudden cessation of alcohol, especially after prolonged use, increases the risk of seizures from alcohol withdrawal. The most typical and severe type of seizure that happens is called tonic-clonic seizures, also called convulsions.
It’s estimated that 2 million Americans suffer the symptoms of alcohol withdrawal every year. Generalized tonic-clonic seizures are the most dangerous and dramatic element of alcohol withdrawal syndrome (AWS). Up to one-third of people with significant alcohol withdrawal may experience alcohol withdrawal seizures.
Free by the Sea can assist with alcohol addiction treatment in Ocean Park, Washington.
What Is An Alcohol Withdrawal Seizure?
The tonic-clonic seizure is what most people think of when they hear the word “seizure.” This type of seizure used to be known as “grand mal” but that term is no longer used. The name “tonic-clonic” comes from combining the characteristics of tonic and clonic seizures. Tonic means stiffening, and clonic means rhythmical jerking. These usually occur within 48 hours of the last drink but could occur at any time during the first week of withdrawal.
This is a tonic-clonic seizure:
- The tonic phase appears first:
- This type of alcohol withdrawal seizure generally begins on both sides of the brain, however, it can start on one side and spread to the whole brain.
- All of the muscles become stiff.
- The air being forced through the vocal cords causes a cry or groaning sound.
- The individual loses consciousness and falls.
- They might bite their tongue or the inside of their cheek. In this instance, their saliva may look bloody.
- After the tonic phase is the clonic phase:
- The arms and usually the legs start to jerk rapidly and rhythmically, bending at the hips, knees, and elbows.
- The jerking slows and stops after a few minutes.
- Their face may look a bit blue or darkish if they’re having trouble breathing or the seizure goes on too long.
- They may lose bowel or bladder control as the body relaxes.
- The person’s awareness, or consciousness, slowly returns.
- A tonic-clonic seizure usually lasts 1 to 3 minutes and takes longer for the person to recover. The individual may be sleepy, confused, depressed, or irritable after it stops.
- A seizure that lasts more than 5 minutes requires immediate medical help. Call 911.
- If the seizure lasts more than 5 minutes, or there are 3 recurrent seizures in a row without the person regaining consciousness in between is a dangerous condition called “status epilepticus.” Hospital emergency treatment is necessary.
Why Do Seizures from Alcohol Withdrawal Happen?

Seizures from alcohol withdrawal occur due to the sudden cessation or reduction of alcohol intake in individuals who have developed physical alcohol dependence. When someone regularly consumes large amounts of alcohol, their brain chemistry adapts to the depressant effects of alcohol. This adaptation involves changes in neurotransmitter levels, particularly gamma-aminobutyric acid (GABA) and glutamate, which help regulate brain activity.
When alcohol consumption is abruptly stopped, the brain’s chemistry is thrown off balance. The absence of alcohol’s depressant effects leads to an overexcitation of the nervous system, as the brain continues to produce higher levels of excitatory neurotransmitters like glutamate. This hyperactivity can result in alcohol withdrawal seizures, which are sudden, uncontrolled electrical disturbances in the brain.
In recent years, impressive advances have been made in understanding the short- and long-term effects of alcohol on the central nervous system. These advances have presented new insight into the physical processes linked with disease or injury.
Alcohol inhibits NMDA neuroreceptors (neuroreceptors process and transfer information received from the neurotransmitters). NMDA receptors play an important part in regulating brain functions including:
- Breathing
- Learning
- Memory formation
- The ability to move about
Suddenly stopping exposure to alcohol results in the brain being easily roused into a state of excitability or irritability (brain hyperexcitability). This is due to the receptors that were being obstructed by alcohol no longer being obstructed.
Brain hyperexcitability reveals itself as:
- Anxiety
- Irritability
- Agitation
- Tremors
Severe hyperexcitability shows as:
- Alcohol withdrawal seizures
- Delirium tremens (DTs)
The Kindling Effect
Research has indicated that the severity of the symptoms of alcohol withdrawal progressively increases over years of alcohol abuse. Repeated detoxes and relapses increase the likelihood of alcohol withdrawal seizures. This is known as the “kindling effect.” The kindling theory is that every withdrawal incident acts as an irritation to the brain. The accumulation of several of these incidents tends to lower the intensity needed for seizures.
Delirium Tremens (DTs)
If you have a seizure from alcohol withdrawal, it’s more likely that you will develop DTs. DTs are the worst part of the alcohol withdrawal process. Typically, if it’s going to happen, it will start about 3 to 5 days after your last drink and it can be life-threatening. Symptoms of DTs include:
- Sudden and severe changes in your mental or nervous system
- Uncontrollable tremors
- Extreme confusion and hallucinations
- Racing heart or irregular heartbeat
- Elevated blood pressure
- Heavy sweating
- Seizures
- Coma and death
Some Facts About Alcohol Withdrawal Seizures
- When consumed in small amounts, alcohol doesn’t cause seizures. Occasional alcohol intake doesn’t increase seizure activity.
- When alcohol is linked to seizures, it is usually the state of alcohol withdrawal that elicits the seizures, not the drinking itself.
- Binge drinking and alcohol withdrawal can even cause status epilepticus, a potentially fatal problem. Binge drinking means 5 or more drinks on one occasion for a male or 4 or more for a female.
- Further studies have shown that alcoholism, or chronic alcohol abuse, is associated with the development of epilepsy in some people. This implies that repeated alcohol withdrawal seizures may make the brain more excitable.
- This points to the possibility that people who have experienced seizures prompted by binge drinking may begin to experience unprompted epilepsy seizures regardless of alcohol use.
Treatment for Alcohol Use Disorder (AUD)

Detoxification (detox) and alcohol withdrawal symptoms are best handled with the aid of medical professionals. This is particularly true if you have a severe or long-term addiction to alcohol. It’s important to physically clear your body of alcohol as much as possible before entering a treatment program. During a treatment program, you will learn to cope with the psychological effects of addiction.
Detox Goals
Alcohol detox is a crucial step in managing alcohol withdrawal symptoms, which can range from mild alcohol withdrawal to severe alcohol withdrawal. For those experiencing mild alcohol withdrawal, symptoms it can be managed with supportive care. However, in cases of severe or complicated withdrawal, which can include seizures, hallucinations, and alcohol withdrawal delirium tremens, medical intervention is necessary to prevent life-threatening complications and ensure a smoother recovery process. The American Society of Addiction Medicine lists three immediate goals for detox:
- To provide a safe place to manage alcohol withdrawal symptoms and allow the individual to become free of drugs
- To provide compassionate alcohol withdrawal care and protect the person’s dignity
- To prepare the patient for further treatment of their dependence on alcohol or other drugs
Medications
- Benzodiazepines–are widely considered to be the drugs of choice to treat alcohol withdrawal and to prevent seizures.
- Haloperidol–may be given for DTs that don’t respond to benzodiazepines
- Beta-blockers–help reduce physical withdrawal symptoms and anxiety
- Clonidine–improves pulse and blood pressure
- Acamprosate–helps maintain abstinence
- Disulfiram–causes unpleasant effects when alcohol is consumed
- Naltrexone–blocks the pleasant effects of alcohol when consumed
Addiction Treatment
After detoxing to clear up the physical addiction, it’s important to enter a treatment program to address the psychological addiction. It’s the changes to your brain that need treatment to help you manage your addiction. To accomplish this, evidence-based behavioral therapies are commonly used.
Behavioral Therapies
Behavioral therapies such as cognitive-behavioral therapy (CBT) and dialectical behavior therapy (DBT) are effective in helping people understand how their harmful thinking patterns are harming their lives. CBT helps people learn the skills necessary to cope with fears and worries without turning to alcohol. DBT leans more toward helping people deal with trauma and manage their emotions.
Group and Individual Psychotherapy
During individual therapy, you work one-on-one with a trained addiction therapist to explore any reasons for your alcohol use disorder. Often, people have a mental condition or past trauma that they haven’t even considered. In group therapy, you will work with a group of other individuals in treatment and one or two therapists. Group therapy helps you look at issues from different perspectives, get advice from others who are struggling with addiction, and be held accountable by other members.
Family Therapy
Because addiction affects every member of the family in some way, family therapy is recommended to help mend relationships and educate family members about the disease of addiction. It’s also recommended that family members engage in some type of therapy or support to help them take care of themselves and help them return to “normal” family roles.
Treatment Programs
There are two basic types of treatment programs: inpatient or outpatient. However, there is a range of levels of care to choose from within these two. They are:
- Inpatient or Residential Programs
This is the highest level of care. Patients live at the facility for an immersive, structured experience.
Outpatient programs range in intensity from:
- Partial Hospitalization Program (PHP)
- Intensive Outpatient Program (IOP)
- Outpatient Program (OP)
The difference between these programs is the amount of time spent at the treatment facility, from 7 days per week to just a few hours a day for a few days per week.
Free By The Sea Recovery Awaits You for Alcohol Addiction Treatment
Free by the Sea is a treatment facility located in the state of Washington on 5 acres of beautiful waterfront property. We have professional relationships with detox centers in the surrounding area, making it easy for individuals to begin their recovery with medical detox in Washington state. After detox, our serene setting and our staff of experienced, compassionate professionals can offer you the rest and rehab that you so desperately need and deserve.
Whether you’re in the area or need to get away, contact us today. We would love to help you on your journey. You are not alone in fighting the battle of addiction. We can help you defeat it!
References:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1312739/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6761824/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6084325/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3860472/
https://www.epilepsy.com/learn/types-seizures/tonic-clonic-seizures
https://www.niaaa.nih.gov/publications/brochures-and-fact-sheets/college-drinking
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6761825/
https://www.cdc.gov/alcohol/about-alcohol-use/index.html
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6943828/
https://pubmed.ncbi.nlm.nih.gov/9018026/
https://www.epilepsy.com/learn/triggers-seizures/alcohol
https://www.magonlinelibrary.com/doi/abs/10.12968/gasn.2018.16.5.S23?mobileUi